Typical housing in the rural areas.
The first few days in Mozambique, I walked with one of our health promoters through the villages. I wanted to see if our work was in fact working. We focus on three health issues in Moz: cholera, malaria and HIV.
Our work is in five rural villages near the port city of Beira. My traveling companions and I walked with the health worker from home to home, speaking with the villagers enrolled in our program and observing.
The good news is that the cholera and malaria projects are working. People are sleeping under mosquito nets and they are treating their water with chlorine (bleach) before drinking it.
The bad news is that HIV is getting worse — much worse. Some estimates have it at 70% in these rural areas.
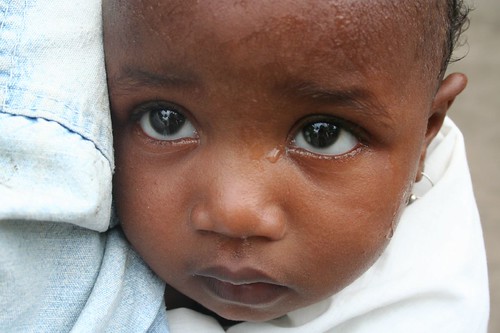
This is the mother of three I wrote about. She is holding her youngest, a one-year-old daughter who is severely malnourished.
Again, I’m not sure what can be done, but I am spending every bit of energy I have at the moment trying to figure something out. There are so many challenges to public health programming when it comes to HIV. You’re essentially trying to get people to change their sexual behaviors, or at least modify them. Politics, religion, economics and culture all play roles in sexual behavior. You can imagine how difficult it is to create one program that works. If changing behavior were easy, all Americans would be thin, we’d wear sunscreen and our seat belts daily and we’d be smoke-free. Point being, getting people to change their routine is very difficult — without the language, cultural, racial and educational barriers I face with this project.
She ate what we had to give — a protein bar.
Back to the books, the research and the conversation. I’m not giving up.
~K